A Report on Medical Workstation Calibration
By Tom Shulte
In years past, the quality of medical images was strictly controlled during the exposure, development, and viewing of hard-copy film. With today’s digital imaging systems, the acquisition of digital images is still tightly controlled, following most of the same practices used for film. However, with modern soft- copy (computer) display systems, image quality control is often neglected during the display and viewing process.
Medical personnel need to know that each soft-copy image they view is an accurate depiction of the tissue and bone that were scanned. The presentation of each image must be repeatable to ensure that every image is shown consistently every time it is viewed. A digital image which has good diagnostic value when viewed on one viewing station should not look different when viewed on another station. This could result in difficulty in reading images, compromised diagnostic value, or even misdiagnosis. Reading difficulty and misdiagnosis due to inconsistent presentation of images can easily be avoided, however, by applying existing technical standards with the medical display calibration tools available today.
Types of Medical Images
There are two broad categories of patient images used in medical practices; radiology images and medical video images.
Radiology images are scanner-sourced images that use some non-visible energy (e.g. X-ray, nuclear, ultrasound, magnetic) to form an interior view of human body parts.
Medical video images are camera-sourced images that use visible light to form a surface view of human body parts or samples. Medical video may be motion video or still video images used in
endoscopy, surgical, ophthalmology, dermatology, and microscopy applications.
Due to differing characteristics between scanner- sourced radiology images and camera-sourced medical video images, there are different performance requirements for displays used to render the two types of images. In the following sections, we first cover aspects of display requirements for radiology imaging. We then cover medical video.
Scanned Radiology Images
X-ray scanning systems are designed to produce image brightness levels that are seen to have a linear relationship to the internal densities of the tissue and bone being scanned. However, these systems produce digital image data that has an approximately logarithmic relationship to the internal densities of the scanned tissue or bone.
The contrast of darker areas of scanned images presented on electronic monitors must be enhanced to achieve perceptual linearity.
If the logarithmic image data produced by these scanning systems were to be displayed on a computer monitor with a logarithmic luminance response*, the monitor would then produce image brightness levels that would be seen to have an approximately linear relationship to the scanned object densities.
*A monitor’s luminance response is the relationship between its digital drive levels (e.g. 0-255) and the resulting screen luminance.
There are two important factors to consider, however, when displaying radiology images on computer monitors.
-
Computer monitors do not natively exhibit a logarithmic luminance response.
- Monitors usually have a luminance response that is approximately a power function, with an exponent (gamma) of 2.2, which is the industry sRGB standard for presenting web and other photographic images. Of course, dedicated medical monitors are initially calibrated with the appropriate luminance response for radiology images.
-
The Human Visual System (HMS) exhibits an approximate logarithmic luminance response over much of its range, but not at lower brightness levels.
- The contrast sensitivity of the HVS depends on factors that include the absolute luminance level, the luminance difference, the ambient lighting environment, among others. Including all factors, human contrast sensitivity is approximately logarithmic above an image luminance of about 20 cd/m2 (Figure 1).
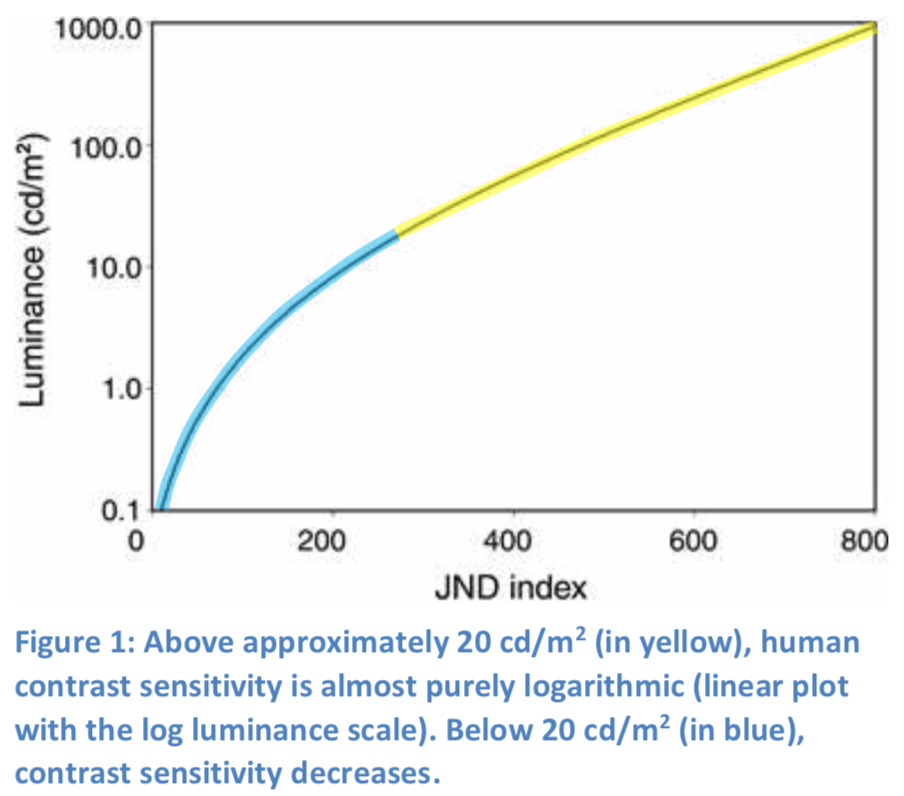
At luminance levels below about 20 cd/m2, however, the contrast sensitivity of the HVS diverges from its near-logarithmic response, with decreasing contrast sensitivity at lower luminance levels (Figure 1).
Thus, the contrast of darker areas of scanned images presented on electronic monitors must be enhanced to achieve perceptual linearity between scanned object densities and image brightness. (Medical films on traditional light boxes produce luminance levels that are mostly above 20 cd/m2 and don’t require this contrast enhancement.)
Therefore, for accurate presentation of scanned images, dedicated medical monitors are initially calibrated with the appropriate luminance response for radiology images. To display radiology images, a monitor’s luminance response should be approximately logarithmic at higher luminance levels, with additional compensation for reduced HVS contrast sensitivity at lower luminance levels.
Inconsistent image presentation from one monitor to another causes inconsistent patient diagnoses and healthcare decisions.
Radiology Imaging Standards
A wide range of monitor types are used to display scanned radiology images that are used for making patient diagnoses and healthcare decisions. Since a given radiology image may be viewed at different locations within a healthcare organization, on monitors with different native characteristics, images produced by the same image file can present completely different visual appearance, information, and characteristics on those different display devices. This inconsistent image rendering from one electronic display to another in different viewing environments, if uncorrected, causes inconsistent clinical perception.
Because the human visual system adapts to overall luminance, different display devices in different locations, with different maximum luminance values, can produce consistent presentation of grayscale images, provided that they have the same luminance ratio and the same luminance response function. This consistent presentation of images across different display devices is the goal of imaging standards for medical radiology displays.
A number of technical standards and practice guidelines for medical imaging digital displays have been developed in the United States over the past 30+ years. Although these standards haven’t had regulatory authority until recently in a few locales, they have been largely accepted by those medical facilities that have implemented quality control programs for their radiology workstations.
DICOM Standard
The American College of Radiology (ACR) and the National Electrical Manufacturers Association (NEMA) formed a committee in 1984 that produced the Digital Imaging and Communications in Medicine (DICOM) standard.[1] Part 14 of the DICOM standard specifies a luminance response model for scanned images known as the Grayscale Standard Display Function (GSDF).
The intent was to cause radiology images to be displayed on any GSDF-conforming monitor with consistent contrast across the brightness range. The DICOM GSDF is the standard luminance response model for viewing scanned medical images. It is designed to produce approximately the same viewing experience on digital monitors that we would experience when viewing radiology film.
The DICOM GSDF matches a monitor’s luminance response to the nonlinear perceptual characteristics of our vision, based on Barten’s model of human contrast sensitivity[2,3]. At luminance levels below about 20 cd/m2, the DICOM GSDF departs from a near-logarithmic model to match the nonlinear perceptual characteristics of the human visual system (Figure 2).
Each equal step in image values should produce a perceptually equal brightness change.
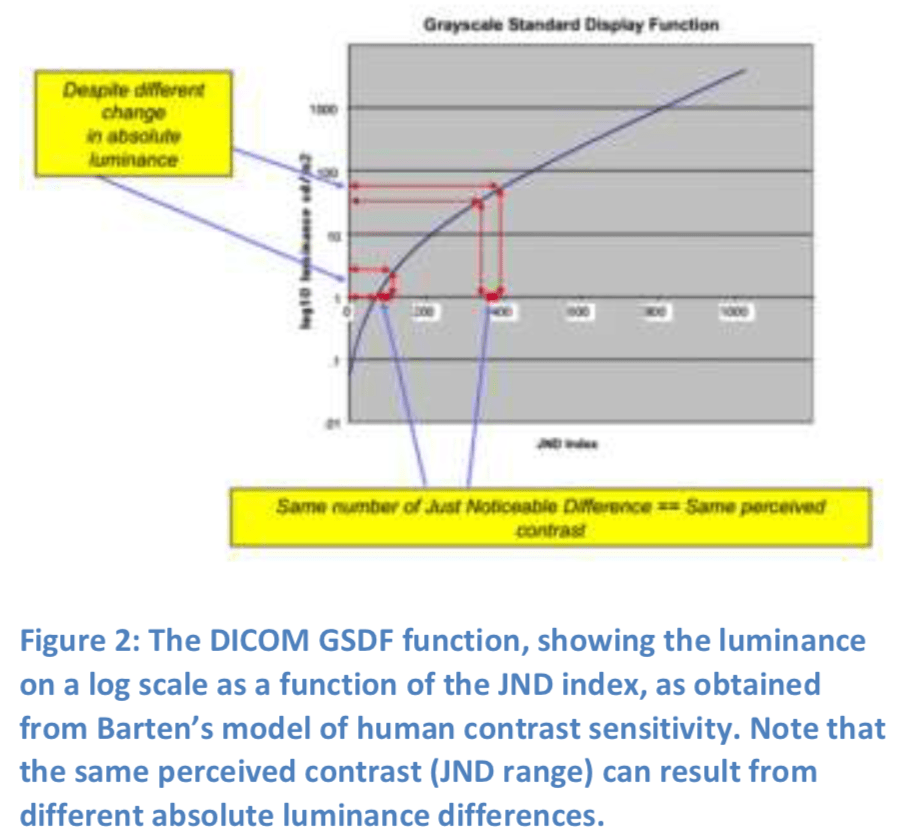
The GSDF maps scanned image values to digital driving levels (signal bit levels), such that equal changes in image values produce equal changes in perceived brightness. The brightness changes are measured in terms of Just-Noticeable Differences (JNDs) of brightness.
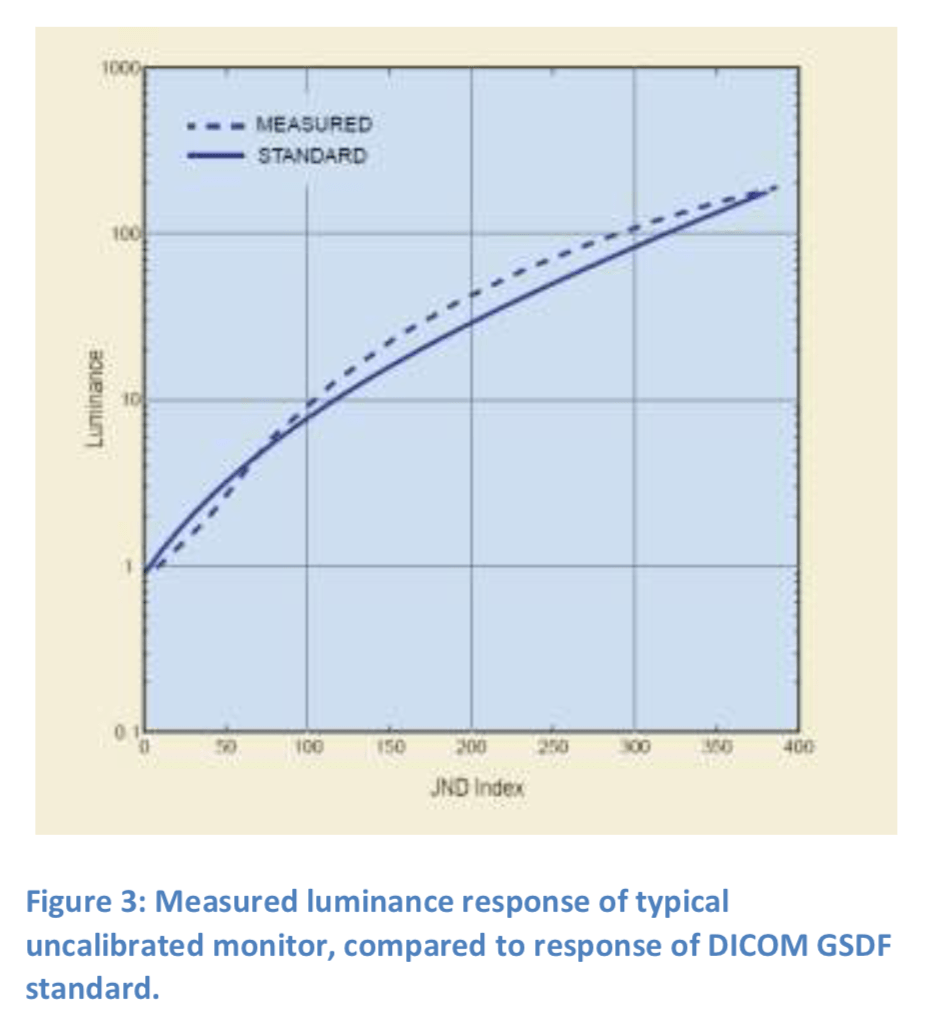
Each equal step in image values should produce a perceptually equal brightness change, across the monitor’s entire luminance range. This equal JND spacing of image brightness steps is called perceptual linearization.
The DICOM Grayscale Standard Display Function (GSDF) ensures that each image level captured by an X-ray scanner is uniquely perceivable on a GSDF- conforming monitor. By standardizing and mapping displays to the contrast sensitivity of the human eye, DICOM calibration ensures that a given difference in gray levels appears the same from one display to the next. This is consistent presentation of images.
Note that the DICOM Standard defines the GSDF luminance response model for radiology monitors, but doesn’t specify any test procedures or acceptance criteria. AAPM and ACR fulfill those needs.
The DICOM GSDF insures that each image level captured by an X-ray scanner is uniquely perceivable on a GSDF-conforming monitor.
AAPM Guidelines
Task Group No. 18 of the AAPM published their On-Line Report No. 03 – Assessment of Display Performance for Medical Imaging Systems[4]. The intent of the report was “To provide standard guidelines to practicing medical physicists, engineers, researchers, and radiologists for the performance evaluation of electronic displays intended for medical use.”
The scope of the guidelines was limited to display devices that are used to display monochrome medical images. The guidelines provide test procedures and tools for evaluating the performance of radiology imaging displays. These include procedures for qualitative (visual) assessments of display performance as well as procedures for quantitative (measured) assessments of display performance.
The guidelines also provide a set of test patterns for the qualitative and quantitative assessments. The TG18 guidelines also recommended quantitative
(measured) QC acceptance criteria that were achievable by CRT displays.
ACR Standards
The American College of Radiology (ACR), in collaboration with the American Association of Physicists in Medicine (AAPM) and the Society for Imaging Informatics in Medicine (SIIM), has published technical standards[5] that, in part, cover radiology diagnostic and clinical displays.
The ACR acceptance criteria for radiology diagnostic, mammography, and clinical displays is covered below, in the Luminance Factors section.
The ACR Practice Guidelines & Technical Standards recommends QC acceptance criteria that are now achievable by LCD displays.
Color in Radiology Images
Although grayscale monitors are most commonly used on radiology reading room workstations, color monitors (both medical and commercial grades) are now being heavily used for clinical workstations and for some diagnostic workstations. The use of color has become significant for clinical images obtained from radiography, ultrasound, nuclear, CT, and MRI, and the color information is being used more and more for decision-making.
Even when color is not required, commercial grade color monitors, rather than medical grade grayscale monitors, are often deployed in primary diagnostic and clinical review imaging stations for purposes of economy. Using color monitors in these formerly grayscale applications does add the need to test for consistent and accurate presentation of both grayscale and color, to not degrade the diagnostic value of either grayscale or color images presented on these color monitors.
Color Standards
There is no standard yet for how color radiology images are to be rendered on medical monitors (as opposed to camera-sourced color medical video images). Medical grade color radiology monitors are calibrated using DICOM GSDF. However, DICOM calibration doesn’t correct a monitor’s color performance. And, DICOM calibration decreases the contrast of camera-sourced color medical video images. As the DICOM GSDF does for grayscale levels, there needs to be a method to create perceptual linearity between color levels in medical images.
Practice guidelines and standards for rendering color on medical displays are being established. Just as the JND metric is currently used to create perceptually uniform grayscale steps, the delta E 2000 color difference metric will be used to create perceptually uniform color steps. DICOM, AAPM, and ICC are currently coordinating efforts to develop methods and standards for consistently displaying color images on medical displays and CalMED is ready to implement those standards.
Luminance Factors
The luminance due to ambient light reflected from a monitor screen reduces the ability to distinguish individual image levels in the darker parts of a scanned image, if the luminance of the darkest image level is close to that of the ambient luminance. The ambient luminance effectively compresses or ‘washes out’ the darker parts of the image and reduces the contrast in the image (Figure 4).
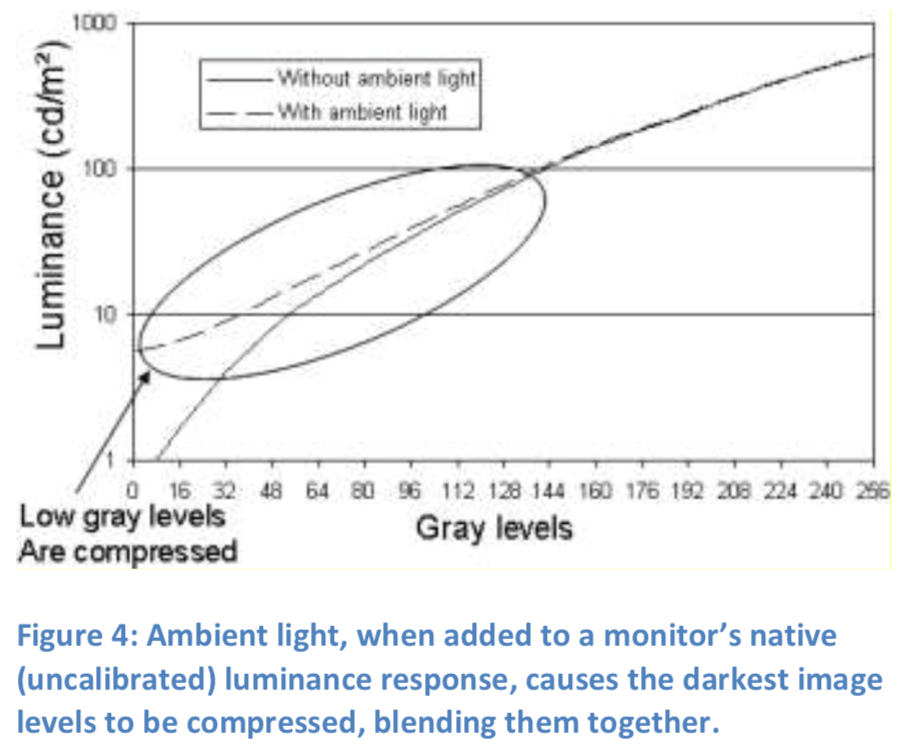
However, a certain amount of ambient room light is required in a reading environment, to avoid eyestrain and to facilitate movement and interaction with other items in the area. It is recommended that about 20 lux of diffuse ambient light be used in diagnostic reading rooms. This is generally sufficient to avoid most screen reflections and still provide sufficient light for the human visual system to adapt to the surrounding environment and the displays.
Minimum Luminance, Ambient Offset
The lowest luminance elements of an image (Lmin) will not be visible if they are darker than the ambient reflected luminance (Lamb). To insure accurate visual perception of all image luminance levels, the luminance produced on a particular monitor by an image’s darkest level needs to be significantly higher than that monitor’s ambient luminance level.
This means that a monitor’s native “black level” normally needs to be increased, to enable accurate perception of the darkest image elements. Because digital RGB monitors don’t usually have a black level control, the image black level needs to be increased before the image pixel values are applied to the monitor as digital drive levels. This is done with a lookup table (LUT) of correction values written to the workstation graphics adapter.
According to the latest ACR technical standards for electronic medical imaging, the lowest luminance level from a scanned image (Lmin) needs to be at least four times the luminance level due to reflected ambient light (Lamb). Also, the lowest image luminance level plus the ambient luminance level (L’min)*, needs to be at least 1.2 cd/m2 for mammography displays, 1.0 cd/m2 for primary diagnostic displays, and at least 0.8 cd/m2 for all other radiology displays.
*The presence of the prime symbol in L’min indicates the inclusion of ambient light.
Note that higher levels of ambient light can be tolerated when viewing medical films on light boxes, because, as noted above, the lowest luminance levels produced by trans-illuminated films are mostly above 20 cd/m2; much higher than the lowest luminance levels produced by computer monitors displaying scanned medical images.
Maximum Luminance
The maximum luminance of a scanned radiology image (Lmax) needs to be high enough to yield sufficient image contrast (JND range) to visually detect each image luminance level difference.
According to the ACR technical standards, a monitor’s maximum luminance needs to be at least 420 cd/m2 for diagnostic X-ray mammography, 350 cd/m2 for diagnostic X-ray radiography, and at least 250 cd/m2 for all other modalities. Multiple monitors on a radiology workstation should have no greater than a 10% difference in maximum luminance between the monitors.
Luminance Ratio
A monitor’s luminance ratio (LR) is the ratio of the monitor’s maximum luminance to its minimum luminance, including ambient (L’min). The monitor’s LR is basically its contrast ratio in the presence of ambient light.
Because the human visual system adapts to the average luminance of a still image, and is not able to optimally adapt to very bright and very dark regions at the same time, we need to limit an image’s overall luminance ratio to a value for which the HVS has reasonably good adapted contrast response. If we reproduce images with a luminance ratio above about 500, no contrast will be perceived in dark regions of the images. If we reproduce images with a luminance ratio below about 250, however, the image will lack sufficient contrast between individual image levels and will appear washed out.
According to the ACR technical standards, a monitor’s luminance ratio needs to be about 350 for optimum contrast (on diagnostic and mammography monitors), and at least 250 for acceptable contrast (on clinical review monitors). The luminance ratio should be consistent on all radiology workstations throughout a medical facility to assure consistent presentation of images.
Note that a monitor’s ability to produce a desired luminance ratio depends primarily on the monitor’s maximum luminance capability, along with its minimum luminance level (increased to compensate for ambient light). Medical and high end commercial
grade monitors will likely be able to produce a suitable luminance ratio, but many commodity- priced commercial grade monitors may have marginal or insufficient maximum luminance (measured in cd/m2, inaccurately called brightness) to produce a desired luminance ratio.
Different display devices can give consistent presentation of images provided that they have:
1. The same luminance ratio (LR), and
2. The same luminance response model (DICOM GSDF).
Bottom Line
Because the human visual system adapts to overall brightness, different display devices, with different maximum luminance values, can give consistent presentation of images provided that they have:
- The same luminance ratio (LR), and
- The same luminance response model (DICOM GSDF).
Grades of Viewing Monitors
RGB monitors of various performance grades are used to view scanned images on radiology viewing stations, depending upon each viewing station’s purpose, be it for primary diagnostic, clinical review, or technologist modality workstation. Monitors used for medical imaging may be purpose-built medical grade monitors or they may be commercial grade monitors. Both purpose-built medical grade monitors and commercial grade monitors are able to fill the needs for rendering radiology scanned images in various use cases.
Commercial Grade Monitors
Commercial grade monitors typically have lower luminance output and no luminance stabilization feature, compared to medical grade monitors. They are typically set to produce their maximum luminance output, typically 200-350 cd/m2, during initial setup. Without automatic luminance stabilization, commercial monitors are unable to maintain constant luminance during backlight warm-up time. When the monitor is first turned on, luminance output tends to be lower until the backlight warms up. They slowly increase to maximum luminance over the first 30 to 60 minutes of run time.
Also, a bright commercial monitor that produces 350 cd/m2 when put into service decays to 250 cd/m2 in about 18 months. Since 250-350 cd/m2 is considered the appropriate luminance range for viewing radiography images, the brightest commercial grade monitors maintain acceptable luminance for only about 18 months.
All monitors used to display scanned radiology images require both initial and annual calibration and periodic conformance testing to insure conformance to industry guidelines.
Medical Grade Radiology Monitors
Medical grade radiology monitors, which are usually used on diagnostic stations in hospital radiology reading rooms, have several features that make them most suitable for use on critical diagnostic reading stations.
Medical grade monitors are generally capable of much higher luminance than commercial monitors, typically producing 300-1100 cd/m2. Medical grade monitors typically have a backlight capable of producing much more luminance than required when the monitor is new. This surplus luminance capability is beneficial because medical grade monitors have a luminance stabilization circuit, with feedback from a backlight sensor, which adjusts the backlight luminance down to the desired output level (250-350 cd/m2).
Since a medical grade monitor has extra initial luminance capability, it adjusts its backlight output to compensate for natural luminance decay, keeping the luminance output constant over time. This backlight feedback circuit is capable of maintaining constant luminance not only over the long term life of the monitor (usually about 5 years), but also in the short term, during monitor warm-up.
An advantage of brighter displays is that they allow radiologists to work in brighter reading environments, reducing viewing fatigue. The display’s minimum luminance should always be regulated, though, to produce the optimum luminance ratio. Per ACR: “For brighter monitors, L’min, should be proportionately larger to maintain the same LR.”
Medical grade radiology monitors may also have a front calibration sensor. The sensor will be integrated with an auto-calibration function within the monitor.
Medical Grade Mammography Monitors
Medical grade monitors designed for viewing mammography images are generally capable of higher luminance than even general radiology medical monitors, some over 1500 cd/m2. This is desirable for displaying mammography images, which tend to be much darker than other X-ray images.
Like general radiology medical monitors mammography monitors have a luminance stabilization circuit, with feedback from a backlight sensor, which adjusts the backlight luminance down to the desired output level (420 cd/m2 for mammography).
The front calibration sensor that is optional on general radiology medical monitors is standard on all mammography monitors. An auto-calibration function within the monitor uses the front sensor for DICOM conformance tests and calibration.
All monitors used to display scanned radiology images require both initial and annual calibration and periodic conformance testing to insure conformance to industry performance guidelines. Medical grade monitors, with their automatic luminance stabilization circuits, usually require quarterly conformance testing and only annual recalibration, while commercial grade monitors may require quarterly or monthly recalibration to assure continued conformance.
Radiology Workstation Test Schedule
Both AAPM and ACR recommend a regular schedule of workstation testing. Following is a typical test schedule that ensures continued compliance to industry standards, high reading efficiency, and no contribution to misdiagnoses due to poor image quality.
Annual Tests – Performed by a medical physicist
- Test ambient lighting
- Calibrate display(s)
- Run integrated calibration software, if available, or
- Calibrate with CalMED software and certified external meter.
- Validate display conformance
- Perform full range tests with test patterns.
- Conformance test with CalMED software and certified external meter.
- Document Results
- Save CalMED conformance report.
Quarterly/Monthly Tests – Performed by a medical physicist or QC tech
- Test ambient lighting
- Analyze display conformance
- Perform luminance response visual tests
(review TG18-QC and TG18-CT patterns) - Conformance test with CalMED software and certified external meter.
- Perform luminance response visual tests
- If poor conformance, calibrate display(s)
- Run integrated calibration software, if available, or
- Calibrate with CalMED software and certified external meter.
- Validate display conformance
- Conformance test with CalMED software and certified external meter.
- Document Results
- Save CalMED conformance report.
Daily/Weekly Tests – Performed by workstation user
- Perform luminance response visual tests
(review TG18-QC and TG18-CT patterns)
Radiology Imaging CalMED Calibration
The Radiology Imaging Technical QC workflow that is provided with CalMED guides us through the process of calibrating a radiology imaging display by implementing industry standard radiology imaging guidelines from DICOM, AAPM, and ACR. An outline of the workflow (Figure 5) is viewable when you open the left hand CalMED panel.
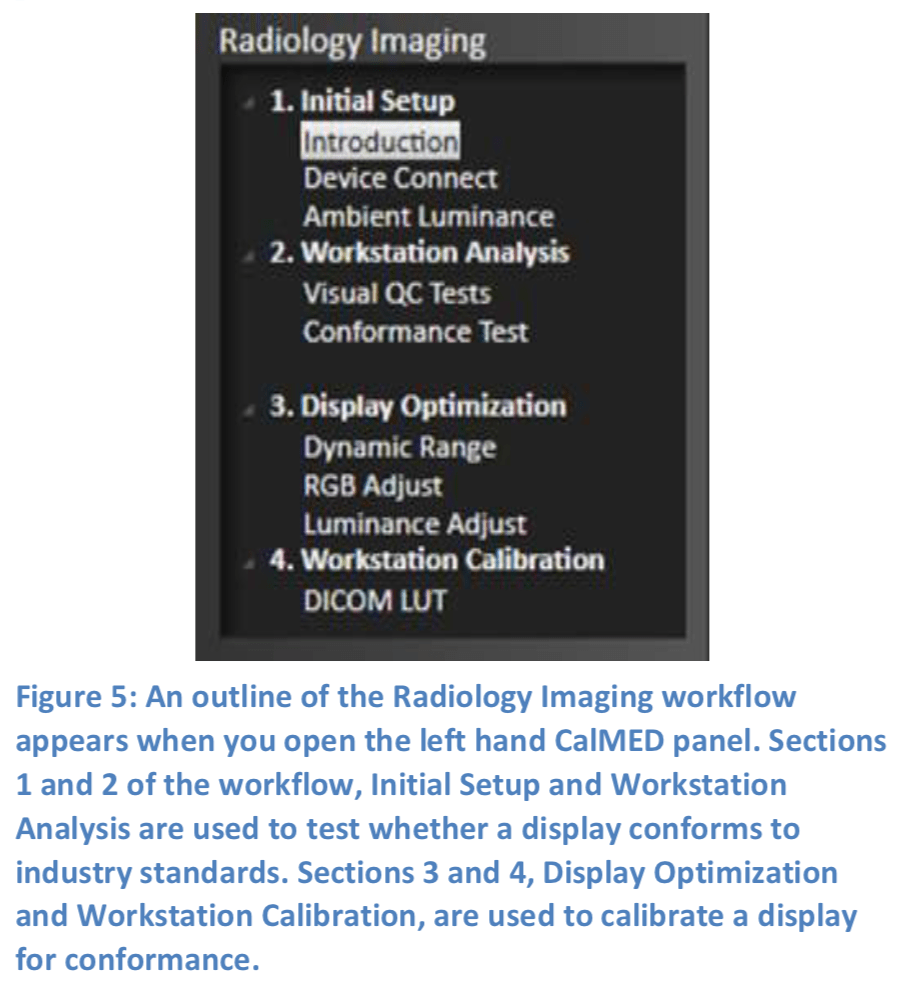
The workflow first guides us through measuring the ambient luminance, setting our minimum luminance target for the display, and then testing the display for conformance to the standard acceptance criteria. If the test shows the display to be in conformance, we can save, view, and/or print a conformance report for the display.
If the conformance test shows that the display is not in conformance, we can then proceed to the additional workflow steps to optimize any controls on the display and then calibrate the workstation. This would be followed by a repeat of the conformance test, to validate and document the display’s conformance to the standard acceptance criteria.
Medical Video Standards
Images viewed on medical video displays originate from cameras, rather than from scanners. These endoscopic and still image cameras are used in surgery, ER, clinics, dermatology and pathology, among others.
Camera-sourced medical images conform to the 1999 sRGB standard from the International Electrotechnical Commission (IEC). Consumer digital cameras and internet images also follow the sRGB standard, which was designed to be appropriate for brighter viewing environments. The sRGB luminance response model starts with a linear section just above black (gamma of 1), then transitions to a power function at higher levels, with a gamma of 2.4. The gamma over the entire luminance range averages to about 2.2.
The sRGB white point (D65) and color gamut (primary colors) are the same as for studio monitors and HDTV.
Medical Video CalMED Calibration
The Medical Video workflow that is provided with CalMED guides us through the process of calibrating a medical video display by implementing the sRGB industry standard. An outline of the workflow (Figure 6) is viewable when you open the left hand CalMED panel.
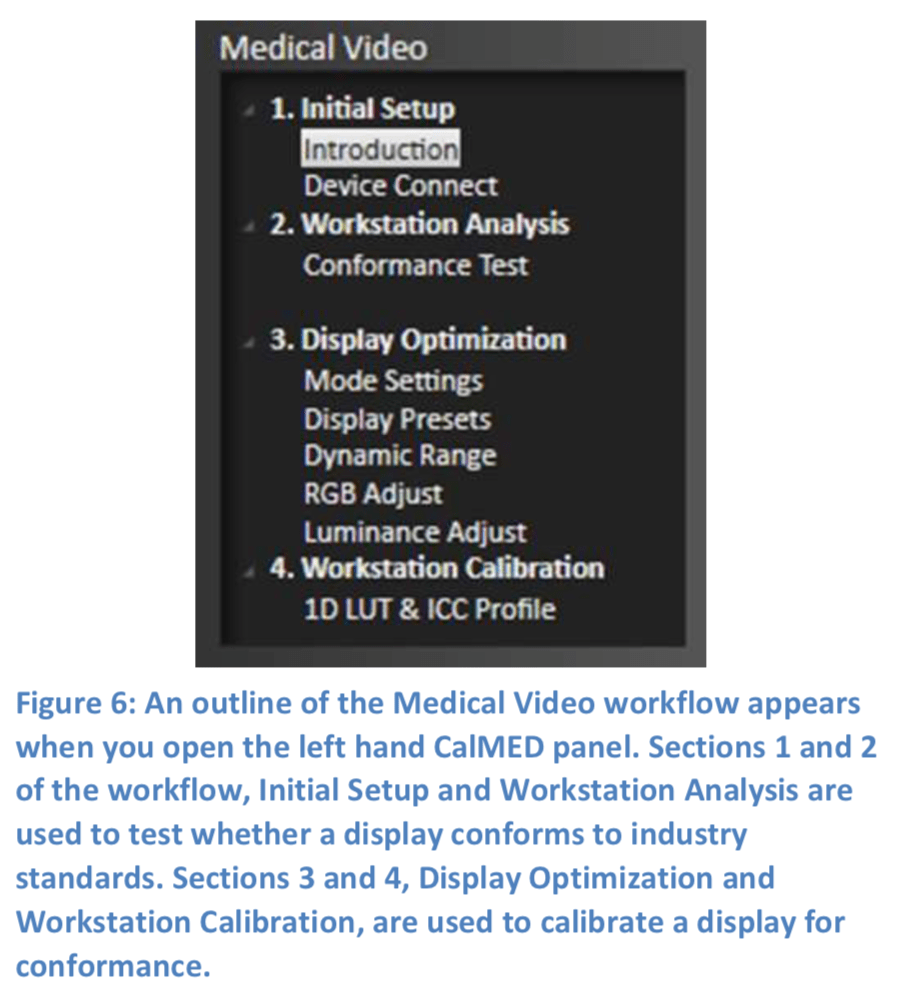
The workflow first guides us through testing the medical video display for conformance to the sRGB standard. If the test shows the display to be in conformance, we can save, view, and/or print a conformance report for the display.
If the conformance test shows that the display is not in conformance, we can then proceed to the additional workflow steps to optimize any controls on the display and then calibrate the workstation. This would be followed by a repeat of the conformance test, to validate and document the display’s conformance to the sRGB standard.
Conclusion
It is critical to provide consistent presentation of medical images, in order to optimize reading efficiency and diagnostic value and to avoid misdiagnoses due to compromised image quality. The medical industry has developed, and continues to develop, technical standards and practice guidelines that follow the characteristics of the human visual system when rendering images on soft-copy electronic monitors.
By maintaining a consistent luminance ratio and luminance response model plus appropriate luminance levels across all displays, you can ensure that medical images will be displayed consistently and accurately on all imaging workstations
throughout a medical network. By maintaining conformance to the appropriate industry standards, both radiology imaging and medical video workstations will consistently render their respective images for efficient and accurate reading.
The CalMED Radiology Imaging and Medical Video workflows provide easy to use processes for routinely testing workstation conformance to standards and, when necessary, provide fast and accurate calibration processes to bring workstations into conformance. Both CalMED workflows provide conformance reports to fully document a workstation quality assurance program.
References
- NEMA: Digital Imaging and Communications in Medicine (DICOM), DICOM PS3.14 2015a – Grayscale Standard Display Function. Available at https://medical.nema.org/medical/dicom/current/output/pdf/part14.pdf
- Barten PGJ. Physical model for contrast sensitivity of the human eye. Proc SPIE Int Soc Opt Eng.1992; 1666: pp57–72.
- Barten PGJ. Contrast Sensitivity of the Human Eye and Its Effects on Image Quality. Bellingham, WA: SPIE Press; 1999.
- Assessment of Display Performance for Medical Imaging Systems, American Association of Physicists in Medicine (AAPM), Task Group 18. Available at https://deckard.mc.duke.edu/~samei/tg18_files/tg18.pdf
- ACR–AAPM–SIIM Technical Standard for Electronic Practice of Medical Imaging, Res. 39 – 2014. Available at https://www.acr.org/~/media/ACR/Documents/PGTS/standards/ElectronicPracticeMedImg.pdf
- ACR–AAPM–SIIM Practice Parameter for Determinants of Image Quality in Digital Mammography Res. 36 – 2012, Amended 2014 (Res. 39). Available at https://www.acr.org/~/media/ACR/Documents/PGTS/guidelines/Image_Quality_Digital_Mammo.pdf